This blog was written by Dr Sheona McHale, Research Fellow, School of Health and Social Care, Edinburgh Napier University 
The study discussed in this blog is funded by the British Heart Foundation.
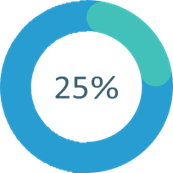 High Blood pressure can increase your risk of having a heart attack or stroke. If you can lower your blood pressure by 10mmHg, you can lower your risk of stroke by 25%. Find out about whether about whether you are at risk of stroke because of your blood pressure here.
High Blood pressure can increase your risk of having a heart attack or stroke. If you can lower your blood pressure by 10mmHg, you can lower your risk of stroke by 25%. Find out about whether about whether you are at risk of stroke because of your blood pressure here.
The COVID-19 pandemic forced changes to healthcare delivery, which particularly affected the management of long-term conditions such as high blood pressure in GP surgeries. Telemonitoring is a way to monitor blood pressure without the need to visit your GP. It allows you to take your blood pressure at home and share your readings with your healthcare team via text or the internet. This is convenient and has been shown to improve blood pressure control.
In our study we wanted to understand how people diagnosed with high blood pressure experienced the delivery of a hypertension service during COVID-19. We were particularly interested in exploring people’s views and experiences of using remote home-based blood pressure monitoring technology and what they thought about going to hospital during the pandemic.
We wanted to learn how people diagnosed with high blood pressure accessed healthcare to manage their condition during a time when routine services were severely disrupted due to COVID-19. Also, we wanted to explore the experiences of patients within NHS Lothian primary care centres who used remote blood pressure telemonitoring to self-manage their high blood pressure during COVID-19 and to compare these to the experiences of patients who did not have access to blood pressure telemonitoring during the pandemic.
We designed a study to gain insight from asking people questions during a telephone interview. The telephone interview allowed us to gain personal views and experiences from high blood pressure patients managed in primary care within NHS Lothian, and who gave their consent to take part in the study.
 We planned to identify and recruit 40 participants via the NHS Research Scotland (NRS) Primary Care Network (20 participants who had experience of telemonitoring technology and 20 without access to telemonitoring technology). Potential participants were identified from clinical records and provided with study information packs. At this point in time, we have not completed the recruitment stage of the study. Upon completion of study recruitment, we aim to analyse the personal views and experiences of participants to help us understand how those diagnosed with high blood pressure accessed healthcare to manage their chronic condition during the C0VID-19 pandemic.
We planned to identify and recruit 40 participants via the NHS Research Scotland (NRS) Primary Care Network (20 participants who had experience of telemonitoring technology and 20 without access to telemonitoring technology). Potential participants were identified from clinical records and provided with study information packs. At this point in time, we have not completed the recruitment stage of the study. Upon completion of study recruitment, we aim to analyse the personal views and experiences of participants to help us understand how those diagnosed with high blood pressure accessed healthcare to manage their chronic condition during the C0VID-19 pandemic.
This study is led by Dr Janet Hanley, Associate Professor, School of Health and Social Care at Edinburgh Napier University. If you would like further information, please contact
Sheona McHale, Research Fellow,
Centre for Cardiovascular Health, Edinburgh Napier University,
Tel: 0131455 3476
Email: s.mchale@napier.ac.uk